Although COVID-19 affects men and women differently, the large majority of current clinical studies of SARS-CoV-2 and COVID-19 makes no mention of sex/gender. Indeed, only a fraction, 4 percent, explicitly plan to address sex and gender in their analysis, concludes a new analysis of nearly 4,500 studies. 21 percent only take this variable into account when selecting participants while 5.4 % go as far as planning to have sex-matched or representative subgroups and samples. The article is published in Nature Communications (available from July 6 at 5pm).
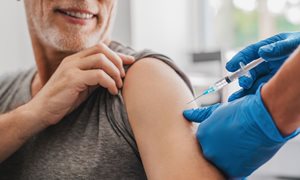
During the corona pandemic, differences can be observed between men and women. Men are more vulnerable to a severe course of COVID-19; more men are hospitalized, and more men die from the effects of the virus. Why that is, we do not know exactly yet, but the consequence of the difference may be that men and women might need different therapies. At the same time, gender is connected to the risk of infection, for example because women more commonly are employed in positions with client or customer contact, or as care-givers, increasing the risk of exposure. This calls for attention to both dimensions in the conduction of clinical trials and planning public health measures.
Still, only a minority of 4,420 registered clinical studies on COVID-19 mention sex/gender in the study registration, a new analysis published in Nature Communications shows. The study is conducted by researchers at Nijmegen's Radboud University Medical Center, Aarhus University, University of Copenhagen and University of Bielefeld.
According to the last author of the article, Sabine Oertelt-Prigione from Radboud University and at the Medical School of the University of Bielefeld, the lacking consideration of sex and gender is problematic: “We have seen from the beginning that the disease does not have an identical course for women and men. The differences in rates of hospitalization and death point to this. This means that our care, such as medicines or other interventions, could also have a different outcome depending on whether the patient is a woman or a man.”
Only 4 percent of studies registered plan to explicitly include sex as a variable in their analysis
The researchers looked at 4,420 COVID-19 studies registered with ClinicalTrials.gov, a U.S. database of more than 300,000 studies from 200 countries. In the COVID-19 sample, 1,659 were observational studies, and 2,475 were intervention studies.
Of these 4,420 registered studies, 935 (21.2%) explicitly addressed sex/gender solely as a recruitment criterion and only 178 (4%) mentioned sex/gender as a planned analytical variable. A further 237 (5.4%) planned sex-matched or representative samples (65) or emphasized sex/gender reporting (172). 124 studies (2.8%) focused solely on one sex, with 100 recruiting only female participants and 24 only male ones. Female-only studies mostly focused on the relation between COVID-19 and pregnancy outcomes.
Research under time pressure
A reason for not including data on sex and gender may be that the studies are conducted under high time pressure. Sabine Oertelt-Prigione: “Researchers are sometimes worried that analyzing sex differences in a study might mean more participants and longer recruitment times to reach their targets. Especially in the early phases of the pandemic, they were working under lots of time pressure ”.
Emer Brady, first author of the study and working at the Danish Center for Studies in Research and Research Policy at Aarhus University supplements with: “On the subject of time pressures, we did hope that as the pandemic wore on and more awareness was raised about the sex and gender disparities we would see more of a focus on sex and gender in the study protocols being registered on ClinicalTrials.gov, but that turned out not to be the case. We also looked at the published trials, where the attention to sex and gender was higher, but still only one in four trials accounted for or reported sex or gender in their analyses.”
Oertelt-Prigione emphasizes the importance of sex and genders role in clinical research: “We increasingly see that men and women respond differently to pharmacological interventions. Ignoring this in trials might lead to serious unwanted side effects later. Looking at sex differences has helped us understand the infection better and it will help us understand our treatment options better. Taking into consideration sex differences is an essential step toward more personalized healthcare.”
Publication in Nature Communications
Lack of consideration of sex and gender in COVID-19 clinical studies - Emer Brady, Mathias Wullum Nielsen, Jens Peter Andersen, Sabine Oertelt-Prigione. DOI: 10.1038/s41467-021-24265-8. Available from July 6 at 5pm.
-
Want to know more about these subjects? Click on the buttons below for more news.
More information
Pauline Dekhuijzen

wetenschaps- en persvoorlichter
Related news items