28 April 2020
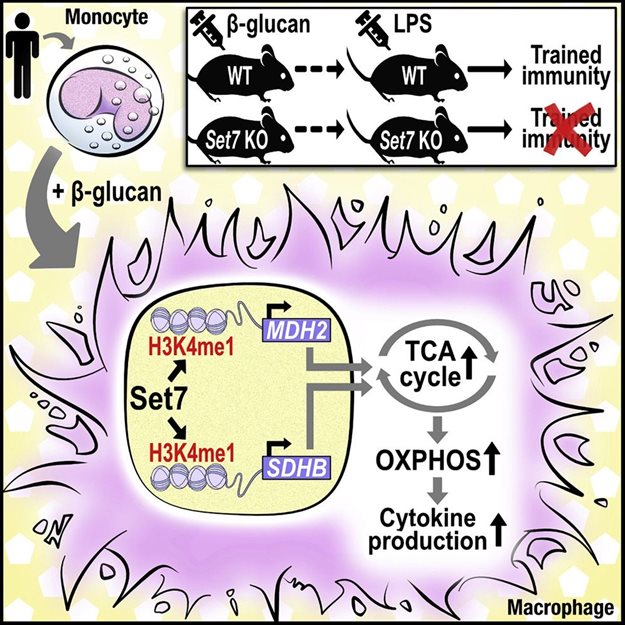
Trained immunity confers a sustained augmented response of innate immune cells to a secondary challenge, via a process dependent on metabolic and transcriptional reprogramming. Previous research from the department of Internal Medicine showed that trained immunity can protect the host against recurrent infections, but can also contribute the pathophysiology in the context of chronic non-infectious inflammatory disorders, such as atherosclerosis. Because of its previous associations with metabolic and transcriptional memory, as well as the importance of H3 histone lysine 4 monomethylation (H3K4me1) to innate immune memory, they hypothesize that the Set7 methyltransferase has an important role in trained immunity induced by β-glucan. Using pharmacological studies of human primary monocytes, they identify trained immunity-specific immunometabolic pathways regulated by Set7, including a previously unreported H3K4me1-dependent plasticity in the induction of oxidative phosphorylation. This finding was validated in vivo in Set7 knock out mice in collaboration with their colleagues from Melbourne.
The identification of Set7 as a key enzyme in the development of innate immune memory provide a potential pharmacological target to modulate trained immunity.

Trained immunity confers a sustained augmented response of innate immune cells to a secondary challenge, via a process dependent on metabolic and transcriptional reprogramming. Previous research from the department of Internal Medicine showed that trained immunity can protect the host against recurrent infections, but can also contribute the pathophysiology in the context of chronic non-infectious inflammatory disorders, such as atherosclerosis. Because of its previous associations with metabolic and transcriptional memory, as well as the importance of H3 histone lysine 4 monomethylation (H3K4me1) to innate immune memory, they hypothesize that the Set7 methyltransferase has an important role in trained immunity induced by β-glucan. Using pharmacological studies of human primary monocytes, they identify trained immunity-specific immunometabolic pathways regulated by Set7, including a previously unreported H3K4me1-dependent plasticity in the induction of oxidative phosphorylation. This finding was validated in vivo in Set7 knock out mice in collaboration with their colleagues from Melbourne.
The identification of Set7 as a key enzyme in the development of innate immune memory provide a potential pharmacological target to modulate trained immunity.

Related news items
COVID-19 associated coagulopathy - lessons after 1 year
17 May 2021 Jenneke Leentjens, Saskia Middeldorp, and colleagues, published a review on the current knowledge of COVID-19 associated coagulopathy and the role of antithrombotic therapies in the Lancet Haematology. go to page
Catecholamines induce trained immunity in monocytes in vitro and in vivo
10 April 2020 Niels Riksen and colleagues contributed data in Circulation Research, to the understanding of pathways driving inflammatory changes in conditions characterized by high catecholamine levels, and proposed that trained immunity underlies the increased cardiovascular event rate in PHEO patients. go to page
Dutch National Postdoc award for Siroon Bekkering
29 November 2019 Siroon Bekkering, theme Vascular damage, will use the prize money (€10,000) for her follow-up research into the memory of the innate immune system of patients with cardiovascular diseases. go to page
RIMLS PhD grants awarded to eight RIMLS (j)PI's
12 September 2019 Recently, RIMLS held an internal call for Radboudumc junior researcher (PhD) positions. Congratulations for all the awardees and all the best in conducting the research projects. go to page
