8 July 2020
Patients who are admitted to the ICU with severe flu infections are also increasingly diagnosed with an infection of the fungus Aspergillus fumigatus. "This is a serious problem," says doctor-microbiologist Paul Verweij, theme Infectious diseases and global health. "Of every five flu patients in the ICU, one gets such a fungal infection. Such an infection is often very serious and associated with a high risk of death."
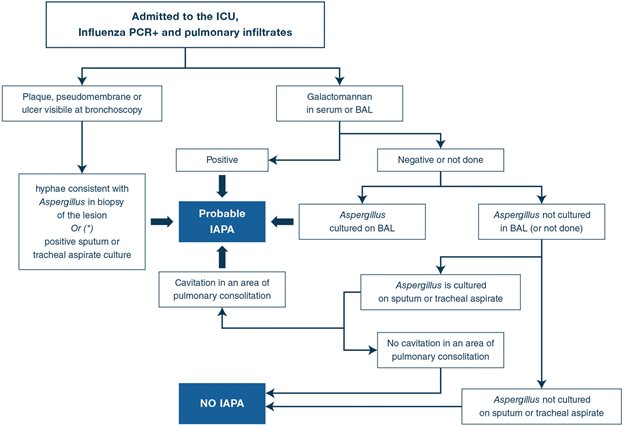
Flowchart of probable IAPA classification. (*)If hyphae consistent with Aspergillus are documented in a biopsy of an airway lesion AND Aspergillus is grown from sputum or a tracheal aspirate, the case fulfills the definition of proven IAPA
Patients who are admitted to the ICU with severe flu infections are also increasingly diagnosed with an infection of the fungus Aspergillus fumigatus. "This is a serious problem," says doctor-microbiologist Paul Verweij, theme Infectious diseases and global health. "Of every five flu patients in the ICU, one gets such a fungal infection. Such an infection is often very serious and associated with a high risk of death."
IAPA
Research into the prevention of such fungal infections after influenza is therefore of great importance. In order to do this properly - also in an international context - a clear definition of this condition is essential and should be used by everyone. In an article in Intensive Care Medicine, six physicians from the Radboudumc, all associated with the Fungal Infections Expertise Centre, and (inter)national colleagues now present such a definition. They call the condition influenza-associated pulmonary aspergillosis, or IAPA for short.CAPA
Just before submitting the article, the new coronavirus that causes COVID-19 suddenly surfaced. Just like the flu, this is a serious respiratory tract infection. Although fungal infections were not immediately reported during the outbreak in China, this link was soon established in Europe. Verweij: "In several countries, including France and Germany, an infection with Aspergillus was also seen in 20 to 30 percent of COVID-19 patients. Therefore, we proposed at the same time a specific definition; CAPA, or COVID-19 associated pulmonary aspergillosis".Definitions important
The importance of a good definition becomes clear when diagnosing the two different disorders. Internist Frank van de Veerdonk, theme Infectious diseases and global health: "Although Aspergillus can cause serious infections in ICU patients with influenza pneumonia, an Aspergillus infection appears to be different in COVID-19 patients. Based on our initial data, the symptoms of an Aspergillus infection appear to be different from those of influenza and the risk of actually developing invasive aspergillosis appears to be lower. Possibly, the fungus often resides in the lungs of COVID-19 patients in the ICU, but without leading to a serious fungal infection, an invasive aspergillosis".Reliable test
This conclusion is not yet entirely certain. A lung wash (BAL) is the most reliable test to determine an infection with Aspergillus in COVID-19 patients. Because of the risks for patient and staff, this test is not commonly applied . If Aspergillus is found in material from the upper respiratory tract, such as sputum, still little is known about the situation deep in the lungs. "But it can also be the other way around," says clinical pharmacologist Roger Brüggemann (theme Infectious diseases and global health) "that is that we find no evidence of an invasive infection in blood, but that the infection is present in the lungs. Especially in the beginning, the antimalarial agent (hydroxy)chloroquine was often used in the treatment of COVID patients. It may also inhibit fungal growth. This may reduce the sensitivity of the Aspergillus test in the blood, so there is a chance that we will find no evidence of an invasive fungal infection in the blood, while the infection is there."More certainty
Because of the diagnostic uncertainty about whether or not invasive Aspergillus infection occurs, the preliminary advice is not to give COVID-19 patients standard prophylaxis (protection) against fungi. Verweij: "But if the clinical condition of the patient gives us cause to do so, we will do so. The aim remains to quickly obtain more certainty through national and international research. The IAPA and CAPA definitions now come in very handy in this search".
Flowchart of probable IAPA classification. (*)If hyphae consistent with Aspergillus are documented in a biopsy of an airway lesion AND Aspergillus is grown from sputum or a tracheal aspirate, the case fulfills the definition of proven IAPA
Related news items

First volunteers vaccinated with Radboudumc malaria vaccine
20 May 2021 Today a new vaccine against malaria, largely developed in Nijmegen, is being tested for the first time in volunteers at Radboudumc. go to page
Trained immunity: a tool for reducing susceptibility to and the severity of SARS-CoV-2 infection
17 February 2021 In a review in Cell Mihai Netea, Frank van de Veerdonk, Reinout van Crevel and Jorge Dominguez Andres propose that induction of trained immunity by whole-microorganism vaccines may represent an important tool for reducing susceptibility to and severity of SARS-CoV-2. go to page
Trained immunity: a tool for reducing susceptibility to and the severity of SARS-CoV-2 infection
29 June 2020 In a review in Cell Mihai Netea, Frank van de Veerdonk, Reinout van Crevel and Jorge Dominguez Andres propose that induction of trained immunity by whole-microorganism vaccines may represent an important tool for reducing susceptibility to and severity of SARS-CoV-2. go to page
Study into better protection for healthcare workers against coronavirus infection
19 March 2020 Radboudumc and UMC Utrecht will investigate whether health care workers are better protected against the coronavirus after a vaccination against tuberculosis (BCG vaccine). This vaccine does not directly protect against the coronavirus, but provides a boost to the immune system. go to page
Two RIHS researchers in top 1 percent by citations
28 November 2019 Bart-Jan Kullberg and Jacques Meis, made it to this year’s list of highly cited researchers. Researchers in this list are selected for their exceptional research performance and are regarded to have had a major impact on fellow scientists. go to page